by James Lyons-Weiler, PhD
© Sept 20, 2021 James Lyons-Weiler Originally published at Popular Rationalism. For more articles by Dr. Lyons-Weiler visit
Del Bigtree and The Highwire Team Noticed an Important Discrepancy Between Public Health Claims and Science that You Need to Know About. Plus: What’s Happening with Memory B-Cells?
One study shows durable and long-lasting active Anti-SARS-CoV-2 neutralizing antibodies following natural infection. Another shows loss of Anti-SARS-CoV-2 neutralizing antibodies in people with prior infection following vaccination. Del Bigtree and The Highwire Team pointed this out in their latest episode – and it’s worth a closer look.
My friends at the Highwire routinely find disparities between public health policy (the “national narrative”, as Del calls it) and science. In their last episode, they showed a mopish Anthony Fauci admit that natural immunity might mean no vaccine for some – and Faucing admitting that he did not have an answer to the question posed by a surprisingly and refreshingly frank Sanjay Gupta. I nearly fell out of my chair the first time I saw this specific interview – Anthony Fauci admitting that he didn’t know something, in and of itself, is noteworthy.
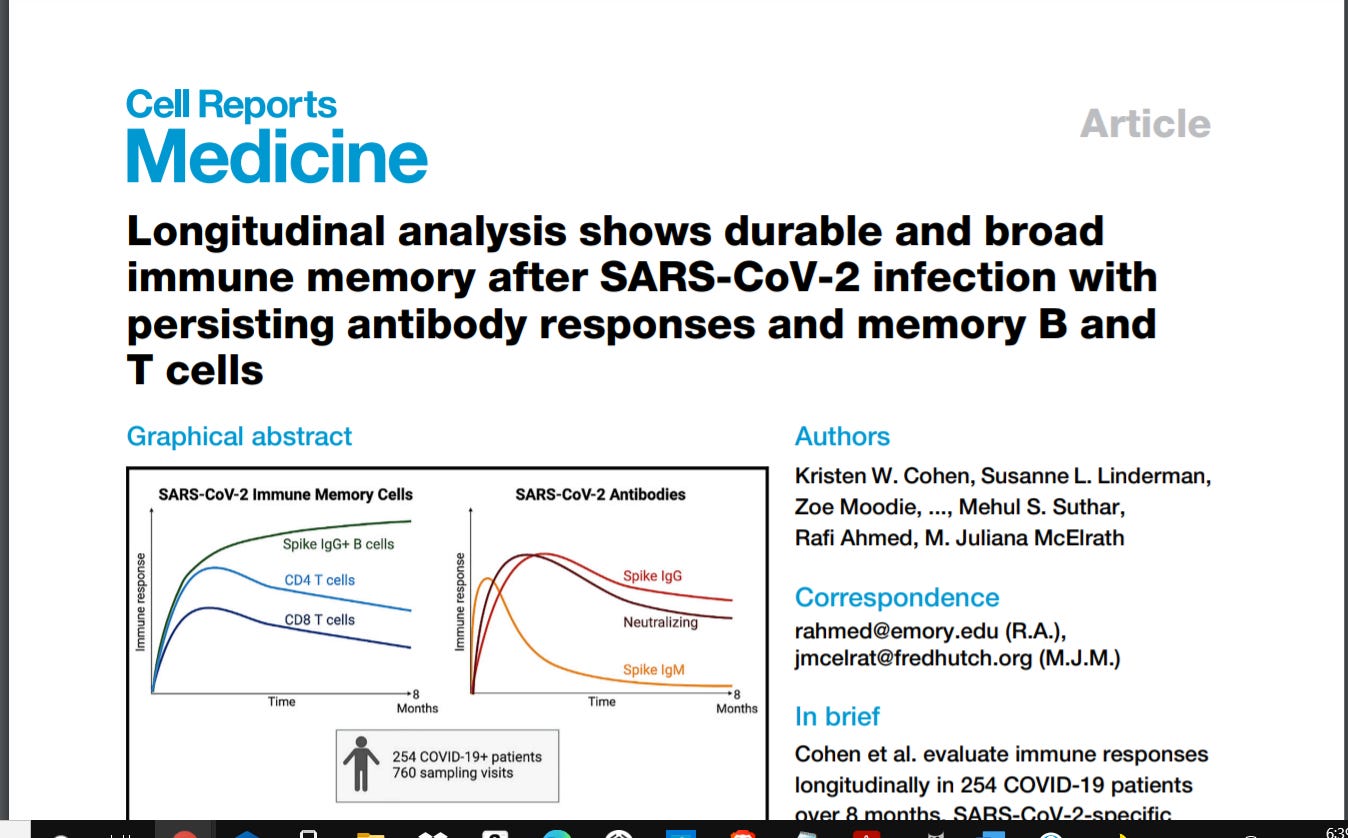
Bigtree then reviews the results of two different studies, which, taken together, do not bode well for COVID-19 vaccine recommendations for the convalescent. The first found “durable and robust” immunity up to 250 days in people who had COVID-19 – a study of which Fauci should have been aware. That study, by Cohen et al., published in Cell Reports, as reviewed by Precision Vaccinations:
“This new study shows that most convalescent COVID-19 patients mount durable antibodies, B cells, and T cells specific for SARS-CoV-2 up to 250 days. The kinetics of these responses provide an early indication for a favorable course ahead to achieve long-lived immunity.”
https://www.cell.com/cell-reports-medicine/fulltext/S2666-3791(21)00203-2
In detail (since numbers matter):
“Of the 183 individuals for whom longitudinal neutralization titers were assayed, 140 (77%) had at least one time point with neutralization titers above the limit of detection (> 20). Seventy-five percent (43/57) of COVID-19 patients generated serum neutralizing antibodies between 30–50 days after symptom onset and similarly 72% (48/67) had measurable titers between 180–263 days after symptom onset.”
So, “efficacy” of natural immunity is 77%; of those 77%, 72% had durable, long-lived neutralizing antibodies of at least 180 and up to 263 days. Note that 72% of 77% is 55.4%. So long-term neutralizing Ab – type immunity from natural infection is 55.4% in the infected, according to this study. Note also that the study looked at Spike, RBD and NTD proteins, and that the two mRNA vaccines in use in the US only target the Spike protein.
The Highwire team pointed out that these results are in stark contrast to the loss of immunity reported in another study, by the Canaday et al. team, which looked at older vs. younger people who had prior COVID-19 infection. Specifically, they examined the effects of vaccination on Spike and RBD neutralizing antibodies in those with natural immunity due to prior COVID-19 who were young healthcare workers with prior infection, (“control group”), and the older NH resident group w/prior infection. The Canaday et al. study found evidence of active Ab immunity at 180 days post-vaccination in the convalescent at rates of only 19% and 35%, respectively.
The comparison of 55.4% (Cohen et al., unvaccinated following COVID-19) to 19% and 35% (Canaday et al., vaccinated following COVID-19) is unexpected and, to put it mildly, worth noting.

It’s worrisome that vaccination appears to deplete neutralizing Abs against the Spike protein gained by infection. It’s puzzling that vaccination appears also to deplete neutralizing Abs against the RBD (receptor-binding-domain) SARS-CoV-2 protein because the vaccines do not target that protein.
A caveat: We have insufficient information on the rates of exposure-produced antibodies in the unvaccinated, vaccine-naive COVID-19 convalescent population compared to vaccine-naive COVID-19 patients who were vaccinated. That would require a human challenge trial, which I think is highly unethical. But it’s unethical to NOT do the animal trials and just presume that people who have previously had COVID-19 can, and should, be vaccinated, given the state of the science on the question. Such studies should use ferrets – and they should look for evidence of disease enhancement and original antigenic sin anew, especially given that the virus has evolved to escape current vaccines.
What About Memory Cells?
It’s also worth noting that T- and B-cell memory immunity were not considered by the latter study – and they are the more important type of immunity when it comes to the question of durability.
Take, for example, an article reviewing available data on immunological decay by Cromer et al.:
The little subfigure in the upper right that shows INCREASES in Memory B-cells – all trending toward 100% of patients – across different studies – proves that we have the ability to store long-term information in our immune systems against the SARS-CoV-2 proteins measured. That’s great news!
We know from other studies that there is a minor, and now we know, temporary “boost” in Ab production in those who have had prior infections following vaccination. These studies are being used to push vaccination in people who have natural immunity. But we don’t know if that “boost” is (a) helpful, or (b) harmful to the entrainment of the immune response to exposure to SARS-CoV-2 in the future. The new data suggest that, in the long run, immunity from natural infection is more durable in the absence of follow-up vaccination. The very bad news is that the current COVID-19 vaccines, designed to address the Wuhan-1 SARS-CoV-2 virus, show weaker and potentially negative efficacy against the Delta variant (e.g., Brackenridge County data). These two realities may be related due to a phenomenon known as “original antigenic sin”, which you can read about here. Or it could be disease enhancement due to pathogenic priming – and given the mangled mess of clinical diagnosis of COVID-19, it’s hard to tell.
For me, two key questions on natural vs. vaccine immunity are:
(1) Since memory B-cells against proteins that are measured by the studies in Cromer et al. show trends toward 100%, can we expect the same for an unknown number of the >50 potential immunogenic targets in the SARS-CoV-2 virus I reported in April, 2020? I think the answer is a strong “Yes!”. That means long-lived, durable and, very importantly BROAD (i.e., redundant) immunity from prior SARS-CoV-2 infection will likely be found to be vastly superior to the narrow immunity attempted by COVID-19 mRNA vaccines, which target only a single antigen source (the Spike protein).
(2) Does vaccination against the single antigen target, the Spike protein, undo the robust and durable – and broad immunologic learning by the memory cells of the human immune system against these other SARS-CoV-2 viral antigens in people who have had COVID-19? I think the answer is “Possibly”, and that studies designed to measure memory B- and T-cell duration that represent long-term immunologic memory against a wide variety of SARS-CoV-2 proteins would be needed to answer that question.
For now, the data on the likely and plausible effects of COVID-19 vaccines on SARS-CoV-2 Spike and RBD protein Ab production from infection are absolutely damning, and this is critical information that should be incorporated into public health policy now.
In short, the data suggest – and the precautionary principle supports – the position that those with prior COVID-19 infections should not be vaccinated until we more fully understand the effects of COVID-19 vaccines on broad, durable, and in some cases hard-won, natural immunity.
 https://thehighwire.com/watch/
https://thehighwire.com/watch/